China Banking Insurance News report 丨 Ensure the health of the aging population, recognize the "three scissors difference"
Since the 1990s, China has changed the public funds for public institutions and labor insurance for enterprises to the current unified social security system. The basic medical insurance system in China has been a self-improving reform that has been "small steps and non-stop" for more than 20 years. process. However, in recent years, with the aging of China's population, under the current basic medical insurance system, more and more elderly people have reappeared in the difficult and expensive conditions. "Blue Book on Ageing: Living Conditions of Urban and Rural Elderly People in China The "Investigation Report (2018)" shows that the elderly have a higher proportion of chronic diseases in China, and the health of the elderly population is only 30% better. In 2017, the elderly's medical out-of-pocket expenses accounted for half of the total medical expenses; medical expenses increased rapidly, far exceeding GDP growth rate. Facing the current situation and new situation of China's population aging, can the existing social security and medical service system continue to improve this contradiction between supply and demand through fine-tuning methods such as cost control and efficiency improvement? The author believes that we must first understand the underlying causes behind the current phenomenon before we can see the true solution. The fundamental reason behind this is that the author believes that there are "three scissors difference" in the current "two methods" (funding methods of basic medical insurance and health care services).
There is a double “scissor gap” in basic medical insurance financing methods
Existing methods of financing basic medical insurance premiums based on wages have increased the proportion of the elderly population, which has led to a decline in the working population and a growing “scissors gap”. The double-digit growth rate and wage growth rate of medical expenses for more than 20 years It also forms a "scissor difference" that cannot be caught up.
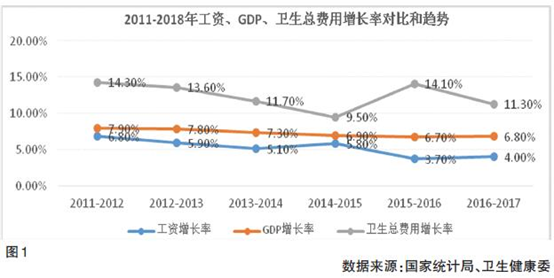
There are hidden dangers in the system of financing in accordance with a fixed wage ratio. The growth rate of total health expenses far exceeds the growth rate of GDP and wages. There is a scissors difference between the method of raising wage bases and the growth of medical expenses far beyond GDP. The "China Social Insurance Development Annual Report 2014" shows that China's personal medical expenditures are already much higher than those of developed countries. The average personal payment of OECD member countries is 10%, while China accounts for 33.2%. Once raised again, the contradiction of expensive medical treatment becomes more prominent. At present, the rate of wage growth cannot keep up with the rate of GDP growth, forming the first risk exposure; the national per capita GDP growth rate in 2011-2012 and 2015-2016 was 7.9% and 6.7% respectively, while the total health expenditure growth rate in the same year was 14.3%. And 14.1%, the growth rate of total health expenditure and GDP growth rate formed the second risk exposure. It is suggested that fees be changed to taxes, and that wages be used as the base to be close to GDP in order to close the first exposure; at the same time, it is necessary to strengthen the control of medical providers and close the second exposure. (See Figure 1)
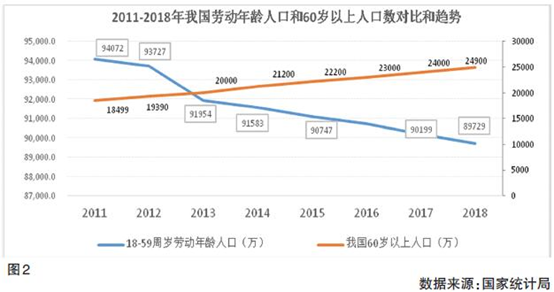
In addition, unlike Singapore, which uses compulsory savings accumulation to meet residents' medical needs, and respects the burden of their own elderly lives, China's current social security financing method is a pay-as-you-go system, which means that working employees pay for retirees. Such an intergenerational transfer-type system design makes it easy for social security reform to begin at the end of the last century, but it will become increasingly stretched in an increasingly aging population. Data from the National Bureau of Statistics shows that from 2013 to 2018, China's 18-59 year old labor population has been declining for several consecutive years. In contrast, the number of elderly people has continued to rise, with a small number of contributors and a large number of users, forming the third Risk exposure. This contradiction between the static financing mechanism and the dynamic population structure has brought tremendous pressure to the sustainable development of medical insurance funds. In response to this problem, if the state's finances allow it, a hard landing can be adopted, that is, the country with historical empty accounts buys out and the newcomers accumulate real accounts. (See Figure 2)
"Scissors difference" in the health medical service system
The resources of the existing medical service system are mainly focused on the diagnosis and treatment of intractable diseases in large top hospitals. This is in contrast to the chronic medical management and health promotion based health medical service systems that are needed by the aging and chronically ill patients. Not the "scissors" of the board.
Chronic diseases have already shown a high incidence in China, and with the increasing number of elderly people in China, the need for chronic disease management is increasing. The "Blue Book on Health Management: China's Health Management and Health Industry Development Report (2018)" states that the number of chronic diseases in China is about 300 million, of which 50% are under the age of 65. The proportion of deaths due to chronic diseases in urban and rural areas in China is as high as 85.3% and 79.5%, respectively. The latest data released by the National Bureau of Statistics shows that by the end of 2018, there were 240 million people aged 60 and over, accounting for 17.9% of the total population. It is expected that the proportion of people aged 60 and over in 2040 will rise from 12.4% in 2010 to 28%. Although the chronic disease management market has hundreds of millions of people's development space, chronic disease medical expenses are high, and chronic disease management services are in short supply, but chronic disease management has always been difficult due to the uneven distribution of medical resources and limited targeted investment. Due to the long-term lack of professional credit and resources for diagnosis and treatment in primary medical institutions, a large number of patients with chronic diseases choose to go to the top three hospitals for medical treatment. The medical resources of the top three hospitals are concentrated in the acute phase of diagnosis and treatment of difficult and severe diseases. Doctors do not have the time and resources to provide chronic disease medical treatment. Health services; For the chronic diseases with high prevalence of the elderly population (a large number of follow-up visits, continuous monitoring, health promotion, etc.), the acute or difficult critical illness diagnosis and treatment resources that are currently good in the medical market of the top three hospitals are out of sync with theirs. More importantly, in the medical service system, there exists a dominant market position of the supply side of "resources drive supply, and supply determines demand". Combining with the "public welfare undertakings" of China's medical system, the hospital's administrative level is high. Status and resource stocks (even increments) are even more difficult to shake. Even trying to "siphon" grassroots customers further, they will not actively adjust themselves and reduce stock resources. This has formed the "fourth risk exposure to ensure the health of an aging population." ". (See Figure 3)
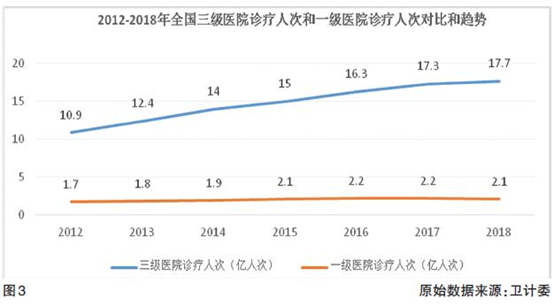
Compared with the high utilization rate of tertiary hospital resources, a large number of primary hospital resources in China are insufficiently used. The bulletin of the Health and Medical Commission shows that from 2012 to 2018, the total number of visits to the tertiary hospitals far exceeded the total number of visits to the first-tier hospitals, and showed a strong upward trend. At present, in the tertiary hospital outpatients, more than half of the patients are patients with chronic diseases, and some of them are in stable condition, and only need to prescribe drugs to maintain routine treatment (re-examination or re-dispensing). Therefore, taking the prevention and treatment of chronic diseases as a breakthrough, changing the people's concept of seeking medical treatment, establishing a scientific and orderly grading diagnosis and treatment system, reasonable flow and appropriateness, can gradually resolve the contradiction between the "overcrowded" and the "difficult to see a doctor" of the city . The structure of health services required by the aging population is different from the resource structure of large hospitals focusing on acute stage diagnosis and treatment. It can be resolved through effective triage. For example, following the objectivity of artificial intelligence triage, eliminating the unreasonable realization of existing medical resources Impulse and reasonable flow promote the adjustment of the stock resource structure. The data shows that 56% of users who think they need emergency treatment choose non-emergency services after using the intelligent pre-diagnosis and triage system; 38% of users who want to go to specialized hospitals choose community hospitals after using the intelligent pre-diagnosis and triage system. Get more convenient medical services. Continuous advancement of graded diagnosis and treatment can also continue to improve the capacity of primary health care services, eventually forming a virtuous circle, and ultimately optimizing and improving the efficiency of medical resource allocation and use.
In short, to ensure the health of the aging population, we must first recognize the "four risk exposures" in the "two ways" and actively face and resolve the "three scissors gap". This is a cross-industry and cross-sectoral For comprehensive system engineering, we need to resolve the scissors gap in the health service system and financing methods through comprehensive management methods such as fee-to-tax reform, medical control and hard landing. Fundamentally in the future, we still need to improve the supervision mechanism of system design in various policies, eliminate short-term behavior of policies, and ensure that we can find executable long-term mechanism solutions; understand the underlying causes and truly solve the aging population's difficult and expensive medical treatment The problem.
This article is reprinted from China Banking and Insurance News: http://shh.sinoins.com/2019-06/05/content_293597.htm

